When your skin breaks out in redness, itching, or blisters for no clear reason, it’s easy to blame soap, laundry detergent, or even stress. But if these flare-ups keep coming back - especially in the same spots - you might be dealing with allergic contact dermatitis. Unlike a simple irritation, this is your immune system reacting to something you touched. And the only way to know exactly what it is? Patch testing.
What Is Patch Testing?
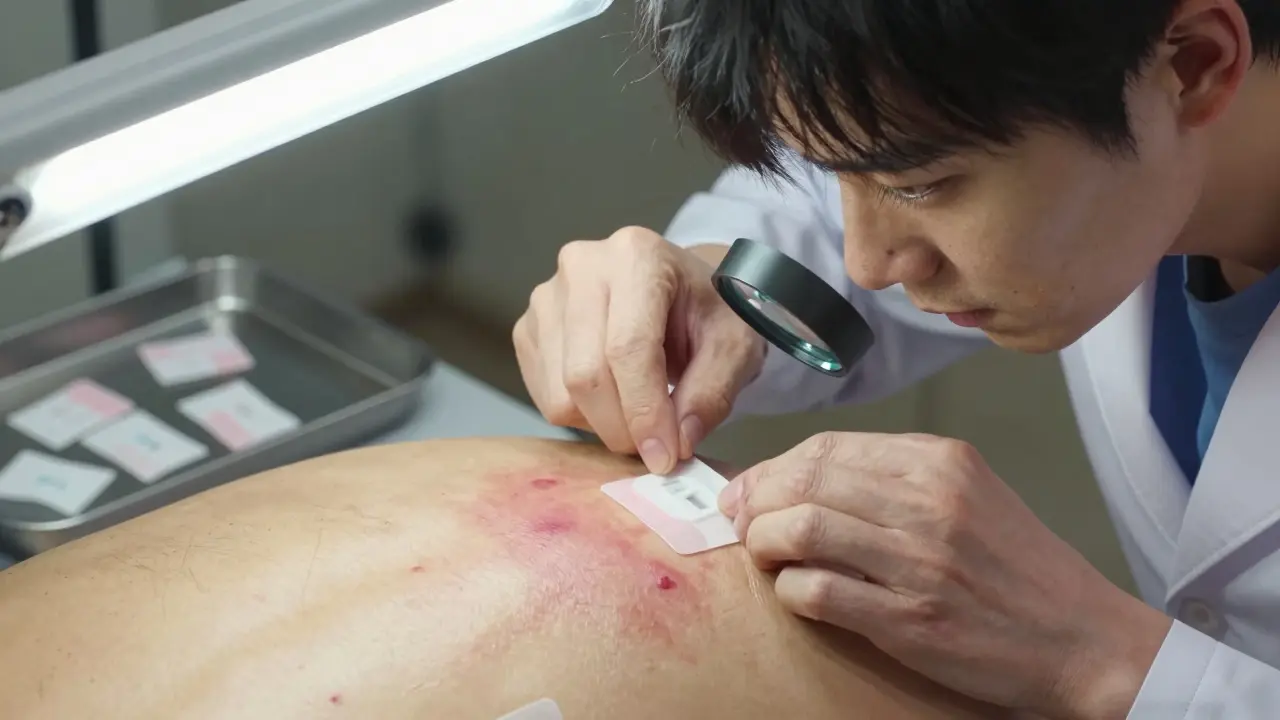
Patch testing isn’t like a skin prick test for pollen or peanuts. Those check for immediate reactions - the kind that make your eyes water or your throat swell right away. Patch testing looks for something slower, deeper, and often more confusing: delayed allergic reactions. These can take two to three days to show up, which is why you don’t just walk in, get pricked, and leave. You come back three times over a week. The test involves sticking small metal chambers - called Finn chambers - onto your back. Each one holds a tiny amount of a different chemical. Between 30 and 100 different substances can be tested at once. These aren’t random guesses. They’re standardized allergens used worldwide, like nickel, fragrances, preservatives, and rubber compounds. The patches stay on for exactly 48 hours. You can’t shower, sweat, or get them wet. No swimming, no hot yoga, no heavy lifting. Even a light rain could mess things up. Then, on day three, you return. The patches are removed, and the skin is checked for signs of a reaction: redness, swelling, tiny blisters. But that’s not the end. You come back again at 96 hours - four days after the patches went on - because some reactions show up late. A positive result means your immune system recognized that chemical as a threat and mounted a response right where it touched your skin.Why Patch Testing Over Other Methods?
Many people think allergy tests are all the same. They’re not. Skin prick tests detect IgE-mediated allergies - the kind that cause hives or anaphylaxis. Patch testing detects T-cell-mediated reactions, also called Type IV hypersensitivity. This is the immune response behind poison ivy rashes, metal jewelry rashes, and reactions to cosmetics. Antihistamines won’t interfere with patch testing. That’s important. If you’re taking them for other reasons - like seasonal allergies - you can keep doing so. You don’t have to stop your meds. That’s not true for other allergy tests. Also, patch testing doesn’t rely on your body’s immediate reaction. It waits. That’s why it’s the gold standard. The American Academy of Dermatology says it’s the most reliable way to find out what’s causing your skin to flare. It’s not perfect. There are thousands of potential allergens out there. The standard test panel covers the most common ones - maybe 70% of cases. But for people with chronic rashes, especially those working in certain jobs, expanded panels are used. Florists might be tested for chrysanthemum allergens. Dental workers get checked for mercury, acrylates, or latex. Construction workers might need testing for epoxy resins or cement compounds. These targeted panels can push detection rates up to 80%.Common Contact Allergens You Might Not Expect
Most people think of nickel - from belt buckles or earrings - as the big offender. And yes, it’s the most common. But here’s what else shows up again and again in patch tests:- Fragrances - Even in “unscented” products. Fragrance mix I and II are standard test items. They’re in lotions, shampoos, deodorants, and cleaning products.
- Preservatives - Methylisothiazolinone (MI) and formaldehyde releasers like quaternium-15. These are in wipes, shampoos, baby lotions, and even some sunscreens.
- Chromates - Found in cement, leather, and some paints. If you’re a builder, mechanic, or gardener, this one hits hard.
- Coconut diethanolamide - A foaming agent in soaps and shampoos. It’s sneaky because it’s labeled as “coconut-derived,” making people think it’s natural and safe.
- Neomycin - An antibiotic in first-aid creams. People use it to treat rashes… and end up making them worse.
- Paraphenylenediamine (PPD) - The main dye in hair color. If you get a scalp or neck rash after dyeing your hair, this is likely why.
What Patch Testing Won’t Tell You
It’s important to know what patch testing can’t do. It won’t tell you if you’re allergic to food. It won’t catch immediate hives or anaphylaxis. And it won’t diagnose irritant contact dermatitis - the kind caused by harsh soaps, detergents, or frequent handwashing. That’s a direct chemical burn, not an immune response. Also, a negative patch test doesn’t mean your rash is “all in your head.” It might be eczema, psoriasis, or another condition entirely. Sometimes, the trigger isn’t in the standard panel. That’s why some dermatologists recommend repeat testing after a few months, especially if your rash keeps coming back. Or they might suggest a “repeat open application test” - putting a suspected product on your forearm twice a day for a week to see if it causes a reaction.What Happens After a Positive Result?
Finding the allergen is only half the battle. The real work begins when you leave the clinic. Avoiding it isn’t always simple. Nickel is in your phone, your jeans buttons, your laptop hinges. Fragrance is in your partner’s body wash, your candle, your fabric softener. Your dermatologist will give you a list of the allergens you reacted to - and their common names. You’ll learn to read labels. You’ll start noticing ingredients like “parfum,” “fragrance,” “methylchloroisothiazolinone,” or “formaldehyde.” You’ll swap out your soap, your shampoo, your lotion. You might even need to replace your leather wallet or your watchband. Topical corticosteroids help calm the flare-ups. Oral antihistamines ease the itch. But the only way to stop the cycle? Eliminate the trigger. That’s why education is part of the treatment. UC Davis Health says it plainly: “Knowing your triggers allows us to guide you in avoiding them and reducing future flare-ups.”

Morgan Dodgen
March 7, 2026 AT 17:29My dermatologist refused to test me for EMF sensitivity. Said it 'isn't real.' But my skin breaks out every time I walk past a cell tower. Coincidence? Or cover-up? 🤨
Stephen Rudd
March 9, 2026 AT 06:14Erica Santos
March 10, 2026 AT 12:32Philip Mattawashish
March 11, 2026 AT 02:24Scott Easterling
March 11, 2026 AT 16:56Mantooth Lehto
March 12, 2026 AT 09:34Mary Beth Brook
March 12, 2026 AT 11:13George Vou
March 13, 2026 AT 05:28Melba Miller
March 13, 2026 AT 18:05Katy Shamitz
March 14, 2026 AT 23:34Nicholas Gama
March 15, 2026 AT 00:55Jazminn Jones
March 15, 2026 AT 10:30Neeti Rustagi
March 15, 2026 AT 22:22Morgan Dodgen
March 16, 2026 AT 16:02Nicholas Gama
March 17, 2026 AT 04:15